1. INTRODUCTION
Matrix metalloproteinases (MMPs) are proteolytic enzymes found to degrade extracellular matrix (ECM) proteins in the human body. They are Zn2+ and Ca2+ dependent endopeptidases comprising 25 different variants. Based on substrate specificity, MMPs are also named as gelatinases comprising MMP-2 and MMP-9, collagenases comprising MMP-1 and MMP-13, membrane MMPs, and stromelysins or MMP-3 [1]. These enzymes are synthesized as zymogens or proenzymes and found to activate on the extracellular membrane [2-4]. The MMPs in normal physiological conditions are involved in angiogenesis, embryogenesis, tissue repair, wound healing, and apoptosis [5,6].
Particularly, normal manifestation of gelatinases (MMP-2 and MMP-9) is considered vital for reproduction, growth, and development of human. The elevated level of these MMPs is found in several pathological conditions such as cardiovascular diseases, cancer, arthritis, pulmonary, and skin diseases [5,7,8]. Earlier studies indicated a correlation between the elevation of MMPs expression and the progression of cervical and ovarian cancers [9-11]. MMP-2 and MMP-9 have been suggested to be linked with the development, invasion, and metastasis of colorectal cancer [12]. Inhibition of MMP-2 and MMP-9 (or gelatinase A and gelatinase B) is a probable way to suppress the growth of cancer and could be an attractive drug target for the treatment of cancer and other MMPs-related disorders [13-15]. Earlier plant-derived compounds with MMPs inhibitory activity have been found to suppress cancer growth without side effects [16-18]. Continuous efforts to identify such active principles from plants will provide natural drug candidates for the treatment of cancers and MMPs-related disorders.
Peltophorum pterocarpum (DC.) Baker ex. K. Heyne is an decorative plant with medicinal values. P. pterocarpum is distributed in the tropical region of the world. The bark of P. pterocarpum is used to treat dysentery, eye disease, muscular pains, toothache, muscular pains, and sores [19]. The flowers extract exhibits cardiotonic, antimicrobial, and antioxidative activity [20]. P. pterocarpum possesses analgesic and cytotoxic effects [21]. The plant extract is also used to treat insomnia and is found to induce good sleep [22]. The active principle compounds such as tannins, triterpenes, steroids, flavonoids, and glycoside were reported from P. pterocarpum [21,23]. Bergenin and C-glucoside isolated from P. pterocarpum were reported to have anti-inflammatory, anti-arthritic, anti-diabetic, anti-HIV, hepatoprotective, anti-arrhythmic, and neuroprotective activities [24-32].
In the present study, an effort has been made for bioactivity-guided fractionation of methanol extract from leaves of P. pterocarpum leading to the purification and identification of active principle compounds with MMP inhibitory activity. Inhibitory assays against MMP-2 and MMP-9 (human recombinant proteins) were executed by in vitro solution assay using azocasein as substrate.
2. MATERIALS AND METHODS
2.1. Materials
Human recombinant MMP-2 and MMP-9, azocasein, and trypsin inhibitor were purchased from Sigma Aldrich, trichloroacetic acid (TCA), silica-gel (mesh size 60–120), NaOH, Tris-buffer, X-ray films, calcium chloride, methanol, chloroform, hexane, and ethyl acetate were obtained from RANKEM, thin layer chromatography (TLC) plates (silica gel 60 F254) procured from Merck, Germany. Purification of compounds was done by high-performance liquid chromatography (HPLC) (Agilent Technologies, Eclipse XDB-C18). The chemicals and reagents used in this investigation were of analytical grade.
2.2. Purification of Bioactive Compounds from P. pterocarpum Leaves
P. pterocarpum leaves were collected in the campus of Dr. Babasaheb Ambedkar Marathwada University, Aurangabad - 431 004 (MS), India. The leaves of P. pterocarpum were rinsed with distilled water twice and dried at room temperature. Using Mixer Grinder dried leaves (2.25 kg) leaves were crushed to fine powder. For preliminary fractionation, the powder was sequentially soaked in n-hexane, chloroform (CHCl3), ethyl acetate (EtOAc), and methanol (MeOH) in the ratio of 1:10 w/v. All extracts were incubated at room temperature (27–28°C) for 10–12 h with recurrent shaking.
The extracts were filtered by cellulosic filter papers and filtrates were further used as the crude source of MMPs inhibitors. On preliminary screening, only ethyl acetate and methanol extracts were found to have inhibitory activity against Clostridium histolyticum collagenase (ChC, sequence similarities to human MMPs) on X-ray film by dot blot assay. MeOH extract exhibited prominent activity and was used for further investigation.
MeOH was evaporated from MeOH extract to concentrate active principles and the final weight of precipitate was 125 g. Half of the MeOH precipitate was dissolved in 1.5 lit of MeOH: CHCl3 (1:9 v/v) mixture for further fractionation, stirred vigorously, and filtered through Whatman filter paper. The solvents from the filtrate were evaporated at their boiling points and 10.4 g of gummy greenish precipitate was obtained. This precipitate was designated as A fraction and subjected to silica gel (mesh size 100–200) column chromatography by applying increasing order of linear gradient of MeOH in CHCl3. Eleven fractions (A1 to A11) were collected and the fractions A1, A2, and A3 were reported to have ChC inhibitory activity. Fraction A3 showing good ChC inhibitory activity (1.94 g) was subjected to silica gel column chromatography and 05 sub-fractions (A3 (1) to A3 (5)) were eluted and analyzed for ChC inhibitory activity. The sub-fraction A3 (4) showed high ChC inhibitory activity further applied to TLC analysis and 03 active principle compounds (compounds 1, 2, 3) were observed. These three active principle compounds were further purified by preparative TLC using a mobile phase MeOH: CHCl3 (2: 8 v/v).
The remaining half of the MeOH extract (powder precipitate, which was not soluble in MeOH: CHCl3 1:9 v/v) was subjected to solid-liquid fractionation with rising order of linear gradient of MeOH in dichloromethane (DCM) in the ratios 2:8 (B fraction), 4:6 (D fraction), 6:4 (E fraction), 8:2 (F fraction), and 10:0 (G fraction) v/v. On screening, fractions F and G showed ChC inhibition. The fraction F was selected for further purification of active principles and applied to silica gel (mesh size 60–120) column chromatography using a linear gradient of non-polar to polar solvents CHCl3, MeOH, and H2O. A total of seven (F1–F7) fractions were collected from the column analyzed for ChC inhibition and fractions F5, F6, and F7 were positive. These fractions were pooled together and subjected to preparative TCL and two active principle compounds (compounds 4 and 5) were purified.
All five purified compounds (compounds 1-3 of MeOH and compounds 4-5 MeOH: DCM) were further subjected to HPLC (Agilent Technologies, Eclipse XDB-C18) for the removal of small impurities. After purification, these bioactive compounds were identified by HRLC-MS and proton nuclear magnetic resonance (1H NMR).
2.3. Dot Blot Assay on X-ray Film
For preliminary screening of MMP inhibitory activity, a dot blot assay or spot test on gelatin-coated X-ray film was performed as described earlier [33,34]. The reaction mixture tubes were contain 5 μL 200 μg/mL ChC (prepared in 50 mM CaCl2 containig 50 mM Tris-HCl buffer pH 7.5), 5 μL 100 mM NaCl, 5 μL buffer, 5 μL of the MeOH extract incubated at 37°C for 10 min. With this one tube was prepared without a MeOH extract and treated as a control. After incubation, tube contents were loaded on X-ray film separately and incubated at 37°C for 15 min. The resulting X-ray film was rinsed with distilled water and air dried. ChC and ChC inhibitors (MMP inhibitors) produced altered patterns of gelatin degradation depending on the potency of the inhibitor, which may be witnessed visually and the resulting X-ray film scanned at 300 dpi using an EPSON scanner.
2.4. In Vitro Inhibition Assay of Bioactive Compounds against MMP-2 and MMP-9
In vitro inhibition of MMP-2 and MMP-9 by purified compounds (compounds 1-3 of MeOH and compounds 4-5 MeOH: DCM) was performed using protein substrate azocasein separately [34,35]. The MMP-2 and MMP-9 activation was performed by incubating Pro-MMP-2 and Pro-MMP-9 with 0.01 mg/mL trypsin distinctly at 37°C for 1 h. Proteoltyic action of trypsin was ceased using 100 μg/mL trypsin inhibitor. In the reaction mixture, 20 μL (120 ng) activated MMP-2 and 20 μL (100 ng) activated MMP-9 (separately), 160 μL buffer (50 mM Tris-HCL pH 7.5, 1 mM CaCl2, 100 mM NaCl and 0.05% Brij-35) and 20 μL (100 μg/mL) purified compound were taken in 1.5 mL centrifuge tubes. After 10 min of incubation at 37°C, 50 μL azocasein (1% w/v) was added to the reaction mixture and incubated for 5 h at 37°C. After incubation, the reaction was stopped by adding 60 μL 5% TCA. TCA soluble peptides (supernatants) were collected by centrifugation at 10,000 rpm for 10 min. About 150 μL supernatant and an equal volume of 1 N NaOH were taken in a microtiter plate. The absorbance was recorded using a microtiter plate reader at 405 nm. Percent MMP-2 and MMP-9 inhibitions were calculated by given that the absorbance of control as 100% MMP-2 and MMP-9 activities separately.
2.5. Identification of Bioactive Compounds
Identification of compounds by high-resolution liquid chromatography-mass spectrometry (HR-LCMS) was carried out at SAIF, IIT Bombay Pawai (MS) India as described previously [36]. Specifically analysis was performed by liquid chromatography coupled with electrospray ionization quadrupole time-of-flight mass spectrometry (LC-ESI-QTOF-MS/MS) Agilent Technologies 6550 i-Funnel system equipped with a G4220B pump, G4226A autosampler and G1316C, and a diode array detector. The 1H NMR spectrum was taken on a Bruker AMX 500 (1H, 500 MHz) spectrometer at Vishnu chemicals laboratories Pvt. Ltd. Hyderabad (MS) India. Metlin database was utilized to analyze structural confirmation.
2.6. Statistical Analysis
MMP inhibitor assays of active principle compounds were conducted with three replicate. Experimental data were analyzed using Microsoft excel 2010. All measured variables were analyzed by one-way analysis of variance (ANOVA) and the variances between the means were related at α value 0.05. The results are presented in the form of bar diagram using mean value ± standard error.
3. RESULTS AND DISCUSSION
MMPs sometimes known as matrixins are responsible for the degradation, repair, and remodeling of ECM components. Although, elevated levels of MMPs are observed in various pathological conditions such as cardiovascular diseases, cancer, arthritis, pulmonary disease, and skin diseases. MMP-2 and MMP-9 are predominant matrixins expressions found to be elevated in various kinds of cancer [12]. The exogenous inhibitors of MMP-2 and MMP-9 of natural origin are drug candidates for the treatment of cancer and other MMPs-related disorders [15]. In this perspective, numerous compounds, namely, flavonoids, alkaloids, and phenolic compounds from plants have shown a promising ability to inhibit MMPs [16-18]. These natural compounds are found to be effective to control MMP-related disorders whereas chemically synthesized inhibitors such as marimastat, doxycycline, and trocade exhibit unwanted side effects [12,37,38]. In the present investigation, we are proposing MeOH extract of P. pterocarpum leaves as a possible source of bioactive compounds with MMP-2 and MMP-9 inhibitory potentials.
3.1. Purification of Active Principle Compounds
Active principle compounds from MeOH extract of P. pterocarpum leaves were purified based on bioactivity assay guided fractionation using silica gel column and TLC. The potential of MMP inhibition was checked at every stage of purification. The fraction with good inhibition toward bacterial ChC was selected. The bacterial ChC shows functions and amino acid sequence similarities with human MMPs [39]. The purity of isolated compounds was assessed by TLC, a single spot appears on the chromatogram when observed [Figure 1].
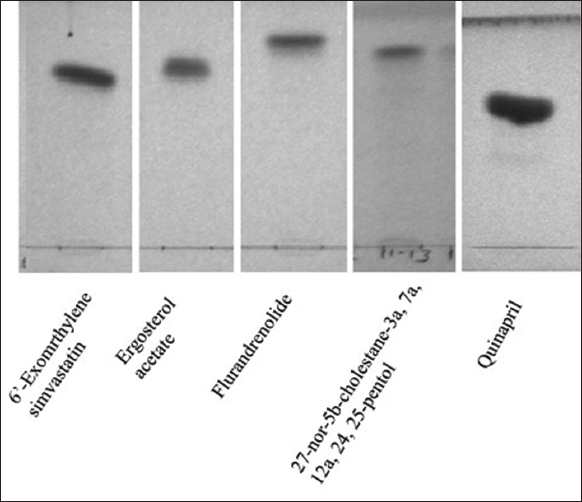 | Figure 1: Demonstration of bioactive compounds of methanol extract of Peltophorum pterocarpum leaves on thin layer chromatography plate. [Click here to view] |
3.2. Structural Properties of Active Principle Compounds
The structures of all purified active principle compounds of methanolic extract of P. pterocarpum leaves are depicted in Figure 2. The structural features assessed by HR-LCMS and 1H NMR are summarized.
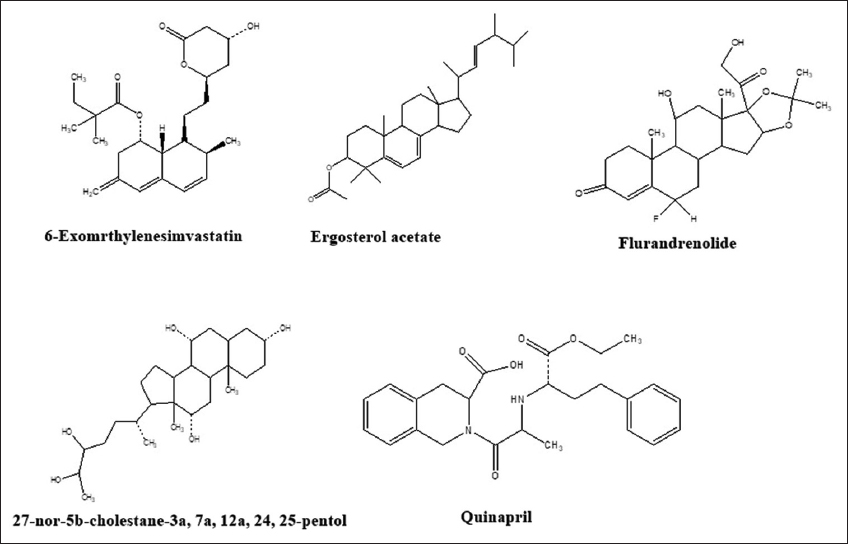 | Figure 2: Structures of bioactive compounds of methanol extract of Peltophorum pterocarpum leaves. [Click here to view] |
3.2.1. Compound 1
6-Exomrthylenesimvastatin was obtained as a whitish colored compound with the molecular formula (C25H36O5) as deduced by HR-LCMS with a matching spectrum to the 1H NMR. Positive-ion ESI MFE m/z 416 [M + H] +. 1H NMR (DMSO) Bruker-300MHz, δ (ppm): 6.96 (s, 2H), 5.89 (s, 2H), 4.96 (d, J = 10.5Hz, 2H), 3.99 (t, J = 9.6, 2H), 3.85(d, J = 10.2Hz, 2H), 3.76 (s, 6H), 3.66 (t, J = 8.7Hz, 3H), 3.50–3.55 (m, 4H), 3.39–3.46 (m, 7H), 3.22 (t, J = 9.3 and 2.4Hz, 4H), 1.65 (s, 2H).
3.2.2. Compound 2
Ergosterol acetate was obtained as whitish colored compound and its molecular formula (C32H50O2) was determined by HR-LCMS with a matching spectrum to the 1H NMR. Positive-ion ESI MFE m/z 466.74 [M + H] +. 1HNMR (DMSO) Bruker-300 MHz, δ (ppm): 6.63–6.73 (m, 1H), 5.81–5.83 (m, 1H), 5.72 (s, 1H), 4.09–4.20 (m, 1H), 3.72–3.89 (m, 6H), 3.66 (d, J = 10.8Hz, 3H), 3.48–3.57 (m, 3H), 3.43 (s, 3H), 2.80–3.19 (m, 5H), 1.84–2.19 (m, 5H), 1.60 (s, 3H), 1.23 (s, 5H), 1.13–1.17 (m, 2H), 1.00–1.11 (m, 6H), 0.93 (s, 2H), 0.87–0.91 (m, 3H).
3.2.3. Compound 3
Flurandrenolide was obtained as whitish colored compound and a molecular formula was assigned as (C24H33FO6) by HR-LCMS with a matching spectrum to the 1H NMR. Positive-ion ESI MFE m/z 436.23 [M + H] +. 1H NMR (DMSO) Bruker-300MHz, δ (ppm): 3.73–3.76 (m, 6H), 3.17 (s, 5H), 2.54 (s, 4H), 2.01 (s, 1H), 1.83 (d, J = 7.5Hz, 2H), 1.56 (s, 3H), 1.23 (s, 4H), 1.15 (t, J = 7.2Hz, 2H), 1.00–1.06 (m, 2H), 0.90–0.93 (m, 1H), 0.85–0.86 (m, 2H), 0.75 (s,1H).
3.2.4. Compound 4
27-nor-5b-cholestane-3a, 7a, 12a, 24, 25-pentol: was obtained as whitish colored compound and its molecular formula (C26H46O5) was determined by HR-LCMS with a matching spectrum to the 1H NMR. Positive-ion ESI MFE m/z 338.6 [M + H] +. 1H NMR (DMSO) Bruker-300MHz, δ (ppm): 4.38–4.75 (m, 12H), 4.12 (s, 1H), 3.63 (s, 4H), 3.51–3.56 (m, 3H), 3.37–3.44 (m, 20H), 3.16 (s, 3H), 2.97–3.03 (t, J = 9.3Hz, 2H), 1.23 (s, 1H).
3.2.5. Compound 5
Quinapril was obtained as whitish colored compound its molecular formula (C25H30N2O5) was determined by HR-LCMS with a matching spectrum to the 1H NMR. Positive-ion ESI MFE m/z 438.5 [M + H] +, 325.09 [M + Na] +.1H NMR (DMSO) Bruker-300MHz, δ (ppm): 8.40–9.30 (m, 5H), 7.97 (s, 1H), 6.77 (s, 3H), 6.34 (s, 2H), 5.50–5.90 (m, 2H), 4.36–4.73 (m, 6H), 3.63 (s, 3H), 3.44 (s, 4H), 3.03 (t, J = 9.3 Hz, 2H), 1.91 (s, 1H), 1.23 (s, 1H).
3.3. ChC Inhibition by Active Principle Compounds
Purified active principle compounds were analyzed for ChC inhibition by dot blot assay on X-ray film. The principle of this method is that when we put ChC (or proteolytic enzymes) on gelatin-coated X-ray film, a transparent blue plastic sheet gets exposed indicating gelatin hydrolysis. This confirms proteinase activity in the control whereas in presence of an inhibitor a dark spot of unhydrolyzed gelatin appeared against the background [40]. We have visually confirmed that all purified active principle compounds exhibited ChC inhibition [Figure 3].
 | Figure 3: Assessment of bioactive compounds of methanol extract of Peltophorum pterocarpum leaves for ChC inhibition by dot-blot assay. [Click here to view] |
3.4. MMP-2 and MMP-9 Inhibition by Active Principle Compounds
Proteolytic activity of MMP-2 and MMP-9 and their inhibition by active principle compounds was assessed by in vitro solution assays. The one-way ANOVA analysis showed that all purified active principle compounds exhibited significant (P < 0.001) inhibitory activities against MMP-2 and MMP-9 [Table 1]. We have observed that quinapril is a potent inhibitor of MMP-2 and MMP-9 displaying 98.21% ± 4.3% and 98.86% ± 3.2% inhibition, respectively. Flurandrenolide exhibited the lowest inhibitory potential against MMP-2 and MMP-9. The 27-nor-5b-cholestane-3a, 7a, 12a, 24, 25-pentol exhibited the highest inhibitory potential (98.28%) while flurandrenolide exhibited the lowest inhibitory potential (63.87%) against MMP-2 [Figure 4]. Inhibitory potentials of all compounds against MMP-2 were observed in order of quinapril (98.21%) ≈ 27-nor-5b-cholestane-3a, 7a, 12a, 24, 25-pentol (98.28%) > ergosterol acetate (80.68%) > 6-exomrthylenesimvastatin (70.38%) > flurandrenolide (63.87%) at 100 μg/mL.
Table 1: One-way ANOVA of the percent inhibition of MMP2 and MMP9.
| Active principle compounds | n | MMP2 | MMP 9 | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Groups | Average | SE | F | P | Average | SE | F | P | |
| Control | 3 | 0 | 0 | 6974 | <0.001 | 0 | 0 | 8374 | <0.001 |
| 6-Exomrthylenesimvastatin | 3 | 71.11 | 0.54 | 72.08 | 0.39 | ||||
| Ergosterol acetate | 3 | 79.63 | 0.53 | 78.90 | 0.43 | ||||
| Flurandrenolide | 3 | 66.59 | 0.61 | 66.20 | 0.53 | ||||
| 27-nor-5b-cholestane-3a, 7a, 12a, 24, 25-pentol | 3 | 97.96 | 0.19 | 82.95 | 0.27 | ||||
| Quinapril | 3 | 97.55 | 0.35 | 96.02 | 0.34 | ||||
ANOVA: Analysis of variance, SE: Standard error.
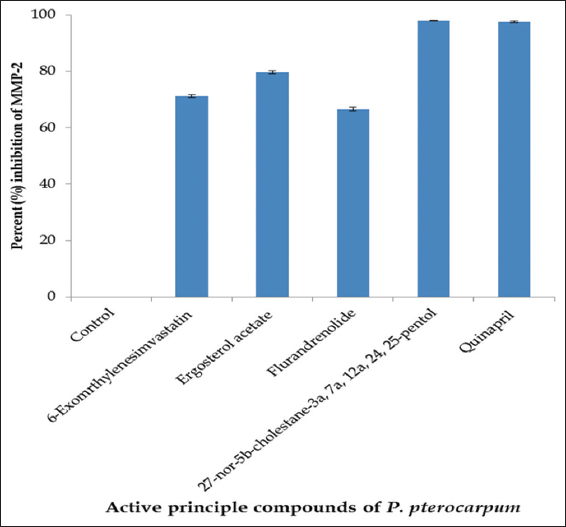 | Figure 4: Assessment of bioactive compounds of methanol extract of Peltophorum pterocarpum leaves for MMP-2 inhibition by in vitro solution assay. [Click here to view] |
Inhibitory potentials of all compounds against MMP-9 were in order of quinapril (98.86%) > 27-nor-5b-cholestane-3a, 7a, 12a, 24, 25-pentol (83.85%) > ergosterol acetate (79.58%) > 6-exomrthylenesimvastatin (72.37%) > flurandrenolide (65.36%) at 100 μg/mL [Figure 5].
 | Figure 5: Assessment of bioactive compounds of methanol extract of Peltophorum pterocarpum leaves for MMP-9 inhibition by in vitro solution assay. [Click here to view] |
Quinapril is an angiotensin-converting enzyme inhibitor and for the 1st time purified from P. pterocarpum leaves [41]. Ergosterol acetate, flurandrenolide, and 27-nor-5b-cholestane-3a, 7a, 12a, 24, 25-pentol are steroidal types of compounds. 6’-Exomrthylenesimvastatin is a statin-like compound. Earlier, it has been reported that the statins are capable to reduce the concentration of MMP-9 in the aortic wall of abdominal aortic aneurysm patients [42]. Simvastatin is a bioactive compound and exhibits anti-inflammatory and anti-atherosclerotic activities in carrageenan-induced female mice [43].
In nutshell, our results indicated that purified active principle compounds of MeOH extract of P. pterocarpum leaves display inhibitory activity against ChC, MMP-2, and MMP-9 could be investigated further in the future for designing or formulating natural drugs for cancer and MMP-related disorders.
4. CONCLUSIONS
This research aimed to identify active principle compounds of MeOH extract of P. pterocarpum leaves with inhibitory potential against ChC and human recombinant MMP-2 and MMP-9. Five bioactive compounds were purified based on bioactivity assay-guided fractionation using silica gel column and TLC. These compounds were identified by HR-LCMS and 1H NMR as quinapril, 27-nor-5b-cholestane-3a, 7a, 12a, 24, 25-pentol ergosterol acetate, 6-exomrthylenesimvastatin, and flurandrenolide. All five active principle compounds showed inhibition against ChC, human recombinant MMP-2, and MMP-9 assessed by dot-blot assay and in vitro solution assays. The identified compounds from P. pterocarpum leaves could be investigated further in the future for designing or formulating natural drugs for the treatment of cancer and MMPs-relevant disorders.
5. ACKNOWLEDGMENTS
The authors are grateful to IIT-Bombay, Mumbai (MS) India, and Vishnu chemicals Laboratory Pvt. Ltd. Hyderabad, India, for the analysis of compounds by HRLCMS and NMR.
6. AUTHORS’ CONTRIBUTIONS
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
7. FUNDING
There are no funding sources to disclose.
8. CONFLICTS OF INTEREST
We declare that there is no conflicts of interest.
9. ETHICAL APPROVALS
This study does not involve experiments on animals or human subjects.
10. DATA AVAILABILITY
All data are available in the manuscript.
11. PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
1. Galis ZS, Khatri JJ. Matrix metalloproteinases in vascular remodeling and atherogenesis:The good, the bad, and the ugly. Circ Res 2002;90:251-62. [CrossRef]
2. Birkedal-Hansen H. Proteolytic remodeling of extracellular matrix. Curr Opin Cell Biol 1995;7:728-35. [CrossRef]
3. Stetler-Stevenson WG, Aznavoorian S, Liotta LA. Tumor cell interactions with the extracellular matrix during invasion and metastasis. Annu Rev Cell Biol 1993;9:541-73. [CrossRef]
4. Chakrabarti S, Patel KD. Matrix metalloproteinase-2 (MMP-2) and MMP-9 in pulmonary pathology. Exp Lung Res 2005;31:599-621. [CrossRef]
5. Dollery CM, McEwan JR, Henney AM. Matrix metalloproteinases and cardiovascular disease. Circ Res 1995;77:863-8. [CrossRef]
6. Zeng F, Cen S, Tang Z, Kang X. Elevated matrix metalloproteinase-9 expression may contribute to the pathogenesis of bladder cancer. Oncol Lett 2016;11:2213-22. [CrossRef]
7. Liotta LA, Tryggvason K, Garbisa A, Hart I, Foltz CM, Shafie S. Metastatic potential correlates with enzymatic degradation of basement membrane collagen. Nature 1980;284:67-8. [CrossRef]
8. Fidler IJ. Molecular biology of cancer:Invasion and metastasis. In:De Vita VT, Hellman S, Rosenberg SA, editors. Cancer:Principles and Practice of Oncology. 5th ed. Philadelphia:Lippincott-Raven;1997.
9. Zhou C, Yao JF, Chen XD. Expression of matrix metalloproteinase-2, 9 and their inhibitor-TIMP 1, 2 in human squamous cell carcinoma of uterine cervix. Ai Zhen 2002;21:735-9.
10. Zhu L, Zheng X, Du Y, Xing Y, Xu K, Cui L. Matrix metalloproteinase-7 may serve as a novel biomarker for cervical cancer. Onco Targets Ther 2018;11:4207-20. [CrossRef]
11. Lopata A, Agresta F, Quinn MA, Smith C, Ostor AG, Salamonsen LA. Detection of endometrial cancer by determination of matrix metalloproteinases in the uterine cavity. Gynecol Oncol 2003;90:318-24. [CrossRef]
12. Mook OR, Frederiks WM, Van Noorden CJ. The role of gelatinases in colorectal cancer progression and metastasis. Biochim Biophys Acta 2004;1705:69-89. [CrossRef]
13. Puricelli L, Dell'Aica I, Sartor L, Garbisa, S, Caniato R. Preliminary evaluation of inhibition of matrix-metalloprotease MMP-2 and MMP-9 by Passiflora edulis and P. foetida aqueous extracts. Fitoterapia 2003;74:302-4. [CrossRef]
14. Mehlen P, Puisieux A. Metastasis:A question of life or death. Nat Rev Cancer 2006;6:449-58. [CrossRef]
15. Vartak DG, Gemeinhart RA. Matrix metalloproteases:Underutilized targets for drug delivery. J Drug Target 2007;15:1-20. [CrossRef]
16. Ferdinando M. Natural bio-drugs as matrix metalloproteinase inhibitors:New perspectives on the horizon?Recent Pat Anticancer Drug Discov 2006;1:91-103. [CrossRef]
17. Chowdhury A, Wei B, Noonan S, Stetler?Stevenson W. Preclinical development of recombinant human tissue inhibitor of metalloprotease?2 as a novel biologic therapy for cancer. FASEB J 2015;29:945-16. [CrossRef]
18. Cabral-Pacheco GA, Garza-Veloz I, Castruita-De la Rosa C, Ramirez-Acuña JM, Perez-Romero BA, Guerrero-Rodriguez JF, et al. The roles of matrix metalloproteinases and their inhibitors in human diseases. Int J Mol Sci 2020;21:9739. [CrossRef]
19. Duraipandiyan V, Ayyanar M, Ignacimuthu S. Antimicrobial activity of some ethnomedicinal plants used by Paliyar tribe from Tamil Nadu, India. BMC Complement Altern Med 2006;17:6-35. [CrossRef]
20. Bairi R, Vijaya C, Ramu A. Evaluation of cardiotonic activity of P. pterocarpum. J Phytopharmacol 2011;2:1-6.
21. Islam MS, Ali S, Rahman M, Islam R, Ali A, Azad AK, et al. Antidiabetic, cytotoxic activities and phytochemical screening of Peltophorum pterocarpum (DC.). K. Heyne root. J Med Plants Res 2011;5:3745-50.
22. Nathan VK, Antonisamy JM, Gnanaraj WE, Subramanian KM. Phytochemical and bio-efficacy studies on methanolic flower extracts of Peltophorum pterocarpum (DC.) Baker ex Heyne. Asian Pac J Trop Biomed 2012;2:S641-5. [CrossRef]
23. Jain SC, Pancholi B, Jain R. Peltophorum pterocarpum (DC.) Baker ex. K. Heyne flowers:Antimicrobial and antioxidant efficacies. Res J Med Plant 2011;5:274-80. [CrossRef]
24. Swarnalakshmi T, Sethuraman MG, Sulochana N, Arivudainambi RA. Notice on the antiinflamatory activity of bergenin. Curr Sci 1984;53:917.
25. De Oliveira CM, Nonato FR, De Lima FO, Couto RD, David JP, David JM, et al. Antinociceptive properties of bergenin. J Nat Prod 2011;74:2062-8. [CrossRef]
26. Chauhan R, Ruby K, Dwivedi J. Himalayan bergenia:A comprehensive review. Int J Pharm Sci Rev Res 2012;14:139?41.
27. Kumar R, Patel DK, Prasad SK, Laloo D, Krishnamurthy S, Hemalatha S. Type 2 antidiabetic activity of bergenin from the roots of Caesalpinia digyna. Rottler Fitoterapia 2012;83:395-401. [CrossRef]
28. Piacente S, Pizza C, De TN, Mahmood N. Constituents of Ardisia japonica and their in vitro anti-HIV activity. J Nat Prod 1996;59:565-9. [CrossRef]
29. Pu HL, Huang X, Zhao JH. Bergenin is the antiarrhythmic principle of Fluggea virosa. Planta Med 2002;68:372-4. [CrossRef]
30. Kim HS, Lim HK, Chung MW, Kim YC. Antihepatotoxic activity of bergenin, the major constituent of Mallotus japonicus, on carbon tetrachloride-intoxicated hepatocytes. J Ethnopharmacol 2000;69:79-83. [CrossRef]
31. Takahashi H, Kosaka M, Watanabe Y, Nakade K, Fukuyama Y. Synthesis and neuroprotective activity of bergenin derivatives with antioxidant activity. Bioorg Med Chem 2003;11:1781-8. [CrossRef]
32. Maduka HC, Okoye ZS, Eje A. The influence of Sacoglottis gabonensis stem bark extract and its isolate bergenin, Nigerian alcoholic beverage additives, on the metabolic and haematological side effects of 2,4-dinitrophenyl hydrazine-induced tissue damage. Vascul Pharmacol 2002;39:317-24. [CrossRef] [CrossRef]
33. Pichare MM, Kachole MS. Detection of electrophoretically separated protease inhibitors using X-ray film. J Biochem Biophys Methods 1994;28:215-24. [CrossRef]
34. Jaiwal BV, Shaikh FK, Patil AB, Hallur RL. Identification of three coagulins as MMP inhibitors from Withania Coagulans dunal fruits. Biomedicine 2022;42:929-37. [CrossRef]
35. Collette T, Bellehumeur C, Kats R, Maheux R, Mailloux J, Villeneuve M, et al. Evidence for an increased release of proteolytic activity by the eutopic endometrial tissue in women with endometriosis and for involvement of matrix metalloproteinase-9. Hum Reprod 2004;19:1257-64. [CrossRef]
36. Tekale SS, Jaiwal BV, Padul MV. Identification of metabolites from an active fraction of Cajanus cajan seeds by high resolution mass spectrometry. Food Chem 2016;211:763-9. [CrossRef]
37. Nelson AR, Fingleton B, Rotherberg ML, Matrisian LM. Matrix metalloproteinases:Biologic activity and clinical implications. J Clini Oncol 2000;18:1135-49. [CrossRef]
38. Provenzano M, Andreucci M, Garofalo C, Faga T, Michael A, Ielapi N, et al. The Association of matrix metalloproteinases with chronic kidney disease and peripheral vascular disease:A light at the end of the tunnel?Biomolecules 2020;10:154. [CrossRef]
39. Eckhard U, Huesgen PF, Brandstetter H, Overall CM. Proteomic protease specificity profiling of clostridial collagenases reveals their intrinsic nature as dedicated degraders of collagen. J Proteomics 2014;100:102-14. [CrossRef]
40. Shaikh FK, Gadge PP, Shinde AA, Padul AA, Kachole MS. Characterization of the AlTI13 protein from Indian siris (Albizia lebbeck) that inhibit the growth of cotton bollworm (Helicoverpa armigera). J Asia Pac Entomol 2014;17:319-25. [CrossRef]
41. Gupta RK, Kjeldsen SE, Krause L, Kneisley J, Posvar E, Weder AB, et al. Hemodynamic effects of quinapril, a novel angiotensin-converting enzyme inhibitor. Clin Pharmacol Ther 1990;48:41-9. [CrossRef]
42. Evans J, Powell JT, Schwalbe E, Loftus IM, Thompson MM. Simvastatin attenuates the activity of matrix metalloprotease-9 in aneurysmal aortic tissue. Eur J Vasc Endovasc Surg 2007;34:302-3. [CrossRef]
43. Carl PS, Charlotte AB, Melba H, Steven M, Heide H, Sushma P, et al. Simvastatin has anti-inflammatory and antiatherosclerotic activities independent of plasma cholesterol lowering. Arterioscler Thromb Vasc Biol 2001;21:115-21. [CrossRef]